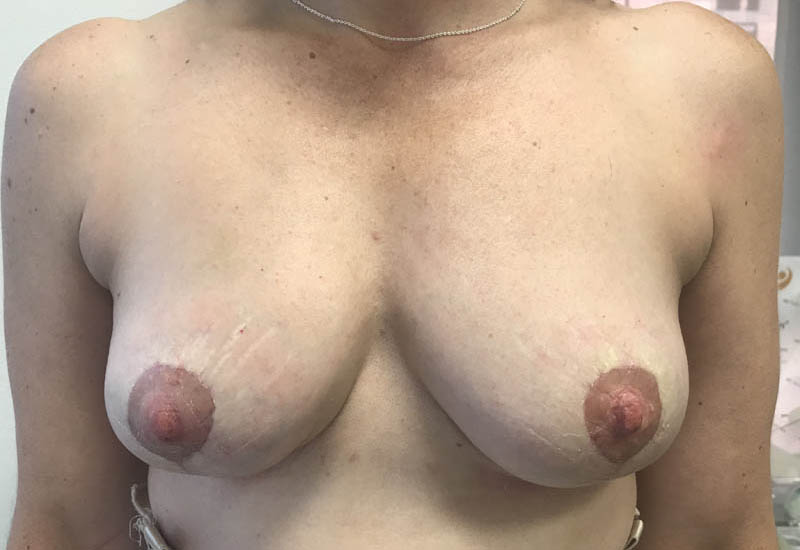
Autologous Fat Graft is using fat removed by liposuction from elsewhere in the body, purified and then grafted in small aliquots to tissue, in order to create regeneration. It is safe to use in the area of cancer treatment and is an extremely useful oncoplastic technique in breast cancer management. Other areas of AFG is in breast aesthetics. Both Breast Lift and Breast Augmentation can be achieved leaving a natural breast appearance, using autologous fat grafting.
Volume improvement of defects with fat grafting is well documented, as in total or partial reconstruction of breast cancer patients. Lohsiriwat et al, demonstrated that adipocyte, preadipocyte and progenitor cell secretion stimulate angiogenesis and cell growth, (Breast, 2011 Aug). Rigotti et al, (Plastic Recontr Surg 2007 April ), demonstrated that lipofilling is more than just a filler – it enhances skin trophicity. He showed that ultrastructure of target tissue systematically exhibited progressive regeneration, including neovessel formation. Treatment with lipoaspirate transplantation led to improvement or remission of the ischaemic nature of the late side effects of radiotherapy. Coleman (Plastic Reconstr Surg 2011 Aug), has recently shown in the murine model, the reversal of fibrosis with fat grafting, and has proposed this mechanism of rejuvenation of fibrotic tissues.
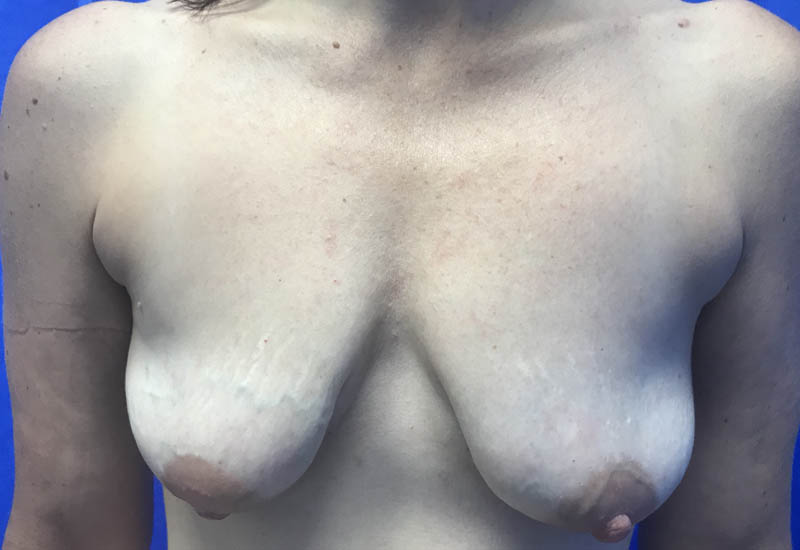
Dr Yap has been using autologous fat grafting extensively since 2012, to improve quality of tissues post radiotherapy, especially contracted defects resulting from the effects of radiotherapy post lumpectomy, as well as in combined reconstructive process with prosthesis post skin sparing mastectomies.
AFG has revolutionised breast reconstruction especially with prosthetic based reconstruction both pre and post pectoral, as well as improved the effects of radiation in these types of reconstruction.
AFG is also useful in treating capsular contracture in both aesthetic and reconstructive procedures.
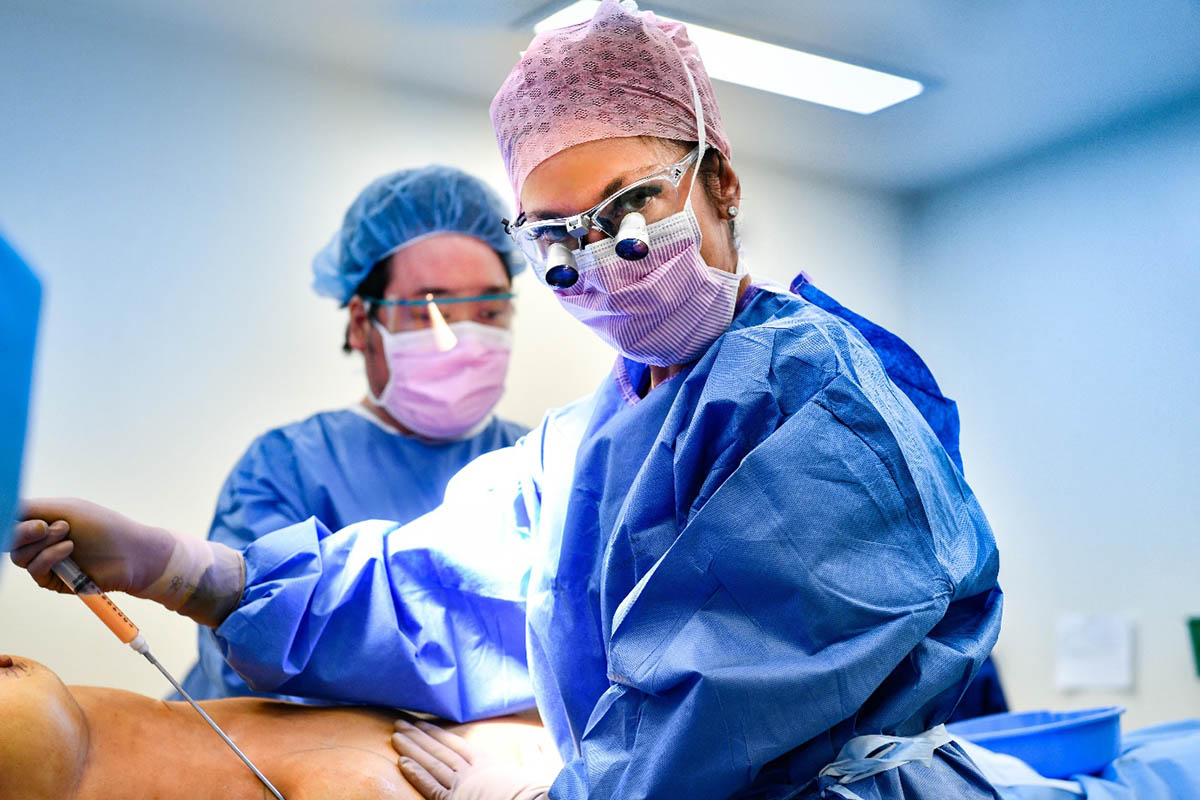
Autologous Fat Grafting Procedure
General Anaesthetic is often performed to reduce the toxic affects of local anaesthetic to the fat cells.
The donor site is best from the thighs and abdomen, but any fat pad area can be used.
Infiltration with adrenaline to donor site reduces bleeding, haematoma, and discomfort post operatively.
Reducing trauma to the fat cells is obtained by using a lower pressure of suction with a 3 mm blunt nosed cannula.
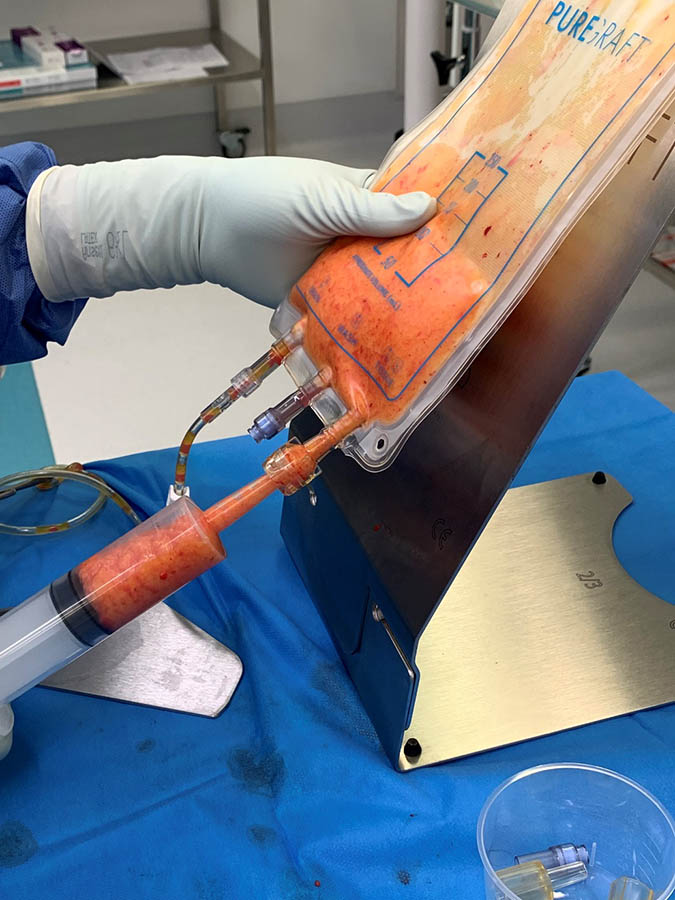
Intraoperative “purification” of fat is created by a process of “washing”, removing impurities, excess oil and blood to leave behind purified fat with its associated stem cells.
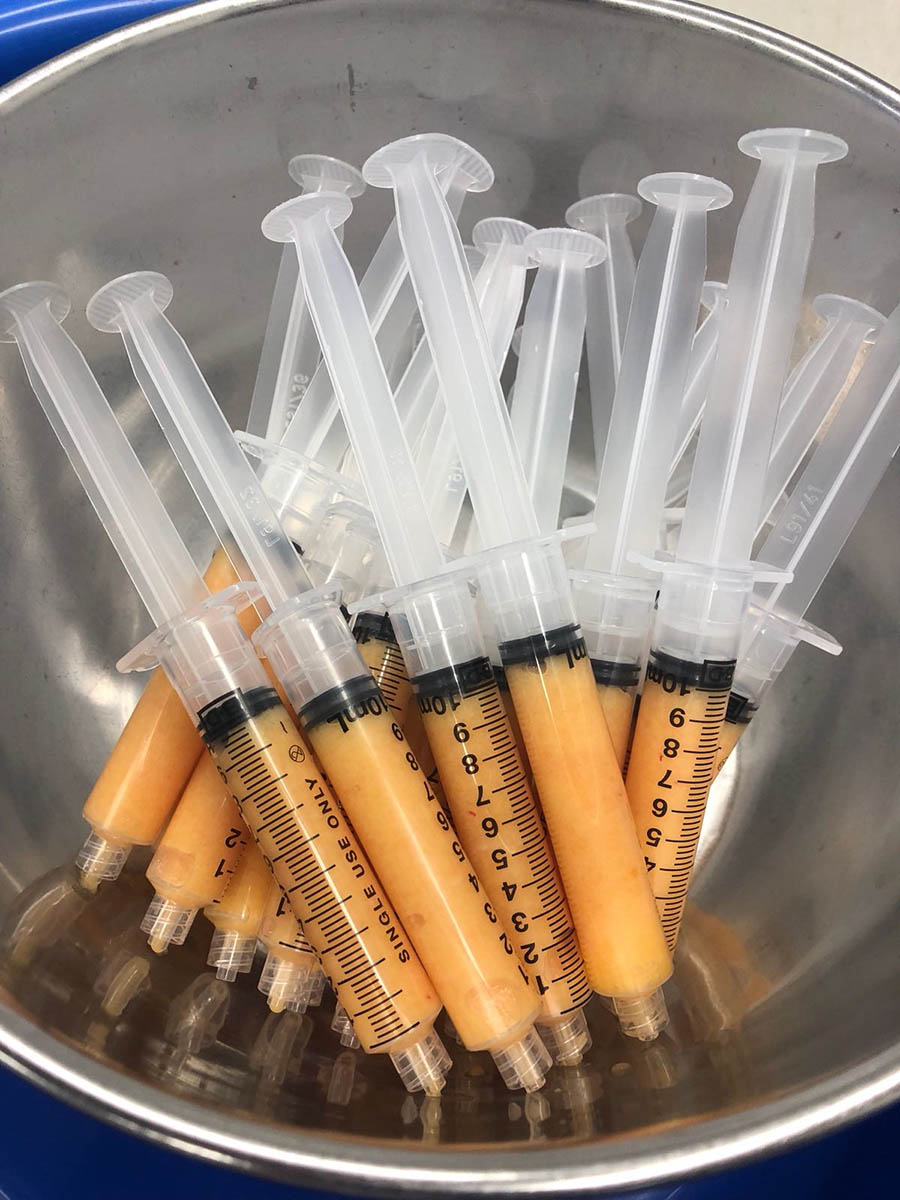
Grafting of fat is performed at multiple tissue planes, delivering small aliquots of fat via a 10 ml syringe, through a 1.8mm blunt nosed cannula.
Complications
- Donor site dimpling if liposuction is too superficial
- Haematoma (blood clot)
- Infection
- Fat embolus (rare)
Result
- Increased volume is achieved but restricted by the amount of well vascularised tissue that can be grafted. On occasion serial grafting may need to be performed in reconstructive cases.
- Serial grafting occurs with a minimum period of 3 months, as regenerating of tissue occurs up to this time.
- Often releasing scar tissue prior to grafting assists with improving contour defects and dynamic affects that can occur with prosthetic based reconstruction.
- Improved trophicity or quality of skin and underlying muscle especially after radiation treatment.