Breast cancer is the second most frequently diagnosed cancer in women, with skin cancers being the most common cancer world-wide. It is expected that 20,000 new cases of breast cancer will be diagnosed in Australia this year. Almost 1% of these will be male breast cancer.
Currently 1 in 7 women will be diagnosed with breast cancer in their life time. Despite the slowly increasing rate, the mortality rates are decreasing which may reflect on increased awareness, leading to earlier presentation, and hence more treatable disease. Breast cancer is the second leading cause of cancer death in women (only lung cancer supersedes it in women). The chance of surviving at least 5 years in the Western world is 91%. The chance that a woman will die form breast cancer is 1 in 39 (2.6%)
Of note, almost 25% of women diagnosed with breast cancer will be less than 50 years of age. Of these, more than 40% is by the age of 40, 20% by the age of 30 and slightly more than 2% by 20 years of age.
Compared to older women, young women generally face more aggressive cancers and lower survival rates. This is because the cancer in the younger age group tends to be biologically more active. This accounts for the incidence of metastatic breast cancer at the time of initial diagnosis, rising in women under the age of 50. Breast cancer is also the most common form of cancer in women who are pregnant or have recently given birth. In the USA, it occurs once in every 3,000 pregnancies, and an estimated 30% or more of all breast cancer in young women is diagnosed in the few years after pregnancy.
Family history of breast cancer, inherited genetic mutations, specifically BRCA1 and BRCA2 must be considered when developing treatment algorithms for all women, specifically less than 50 years of age.
Protective Factors
Exercise and reduced BMI
- Active women have reduced breast cancer risk compared with inactive women.
- Guidelines suggest that at least 30 minutes of moderately cardiovascular intense exercise every day, and muscle strengthening exercise 2 days a week are recommended. This assists with reduction of obesity.
Breast Feeding
- Longer breastfeeding is associated with lower breast cancer risk (12 months or longer)
Relative risk factors in developing breast cancer
Alcohol consumption – This is considered in consumption greater than two alcoholic drinks/day. Alcohol can affect the ability of the liver to control the levels of oestrogen in the blood with may increase risk of breast cancer. It can also increase the risk by damaging DNA in cells and hence leading to cancer.
Smoking and the association with breast cancer is unclear
Personal history of breast cancer increases the risk of developing a new breast cancer in remaining breast tissue
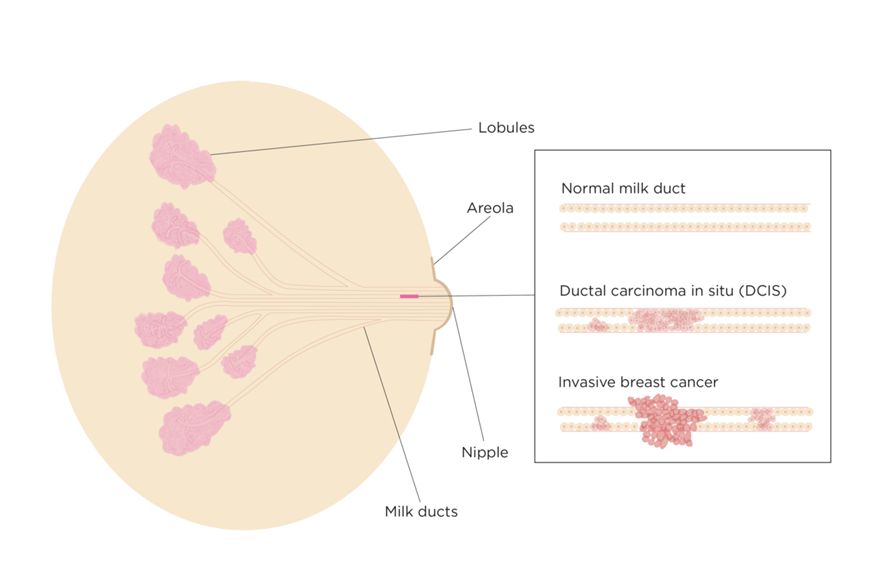
Non invasive conditions – DCIS Ductal Carcinoma in situ (breast cancer cells derived from the milk ducts which have not yet invaded normal tissue) . DCIS is commonly diagnosed incidentally on a mammogram as it does NOT present with signs or symptoms. A diagnosis of DCIS affords a 3.9 times likelihood of a cancer developing.
DCIS is categorised into low, intermediate and high grade. Intermediate and high grade disease is more likely to become a true invasive cancer and should be removed surgically. Depending on the extent of the disease, a wide local excision or mastectomy is appropriate. Radiotherapy can be used on the remaining breast tissue of the affected side to prevent recurrence. Often an anti oestrogen medication is used to help prevent recurrence. These include Tamoxifen and occasionally Aromatase inhibitors
LCIS (Lobular Carcinoma in situ) – LCIS is a non-invasive breast pathology which originates from the lobules which are the milk-producing glands. Presence of LCIS increases the risk of developing an invasive breast cancer.
ADH (Atypical ductal Hyperplasia) ADH is also a non invasive condition but will increase the chance of developing a breast cancer in the area, and so is best removed when diagnosed.
Dense Breast Tissue
The composition of breast tissue is a combination of glandular tissue with fatty and fibrous tissue. With age and change in hormonal levels, the composition changes. Dense breasts are often noted on mammogram, and describe the increased composition of glandular and fibrous tissue, with decreased fatty tissue content.
Women with dense breasts for their age, have an increased chance of developing breast cancer than women with less dense breasts, up to 1.6 times. Dense breast tissue also decreases the sensitivity of the 2D mammogram. 3D and contrast mammography is better for imaging in these groups.
Factors which influence mammographic dense breasts are younger women, low BMI, hormone replacement therapy, and pregnancy.
Radiation Treatment
Radiation to the chest or face as in conditions such as lymphoma treatment
HRT and the Oral Contraceptive Pill
Some studies show that these treatments are a risk factor but it is still under debate.
Breast cancer does not make you feel unwell especially in the early stage
Breast Symptoms
Being breast aware means that each individual woman knows what is “normal” for their breast. Any change from normal should be investigated.
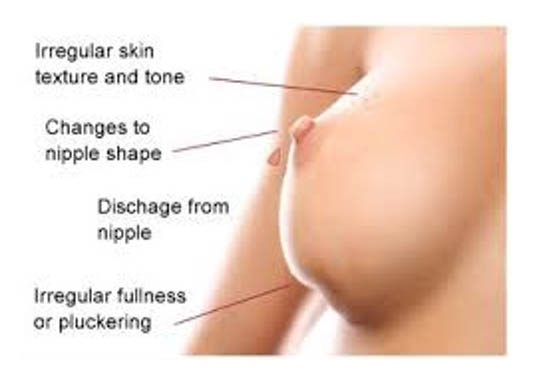
Breast symptoms of concern are:
- Breast lump
- Nipple discharge especially if bloody and only on one side
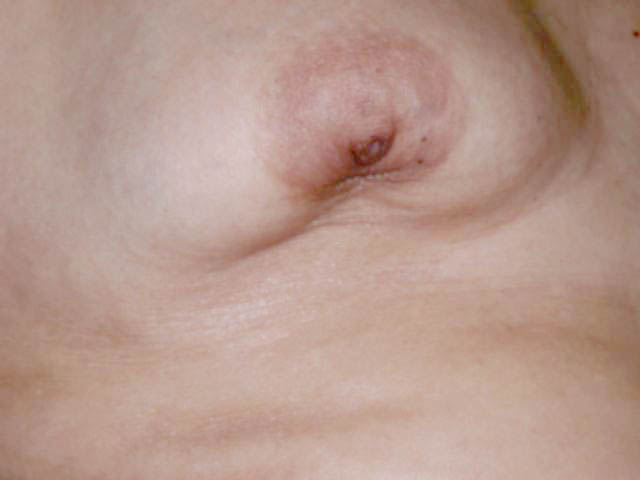
- Nipple retraction
- Skin dimpling
- Breast pain (less common in breast cancer)
- Skin changes such as thickening, eczematous changes especially around the nipple-areolar complex
Diagnosis
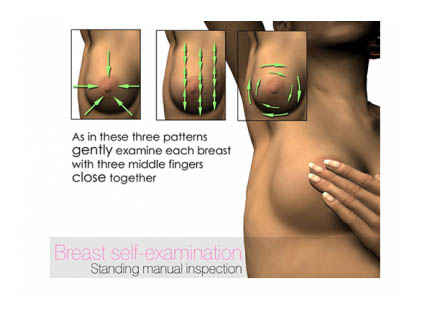
Breast self-examination is important at regular periods. The best assessment is in the shower using soapy lather, with the pads of at least two fingers. This is best performed in premenopausal women, during the midcycle when breast tissue is less active.
The assessment of breast symptoms should be a “triple assessment”, with the health professional performing a clinical examination, followed by imaging of both breasts.The imaging should be both a Mammogram, and a bilateral breast Ultrasound.
Mammography should be performed in any age group as it is the best form of imaging for finding DCIS (ductal carcinoma in situ), a precancer condition. In the age groups less than 50 year, or those women with dense breasts, a 3D mammogram is better at analysing the tissue.
Findings indicative of Malignancy:
- Stellate appearance and spiculated border
- Microcalcifications
- Lobulation, architectural distortion
A normal Mammogram DOES NOT rule out suspicion of cancer based on clinical findings.
Breast Ultrasound is particularly good at assessing solid and cystic (fluid filled) lesions. In ages less than 40 years, it can have a false negative rate of up to 10%. This means that these lesions which are breast cancers have benign features on ultrasound up to 10% of the time, and therefore all new palpable lumps should be considered for biopsy.
Magnetic Resonance Imaging (MRI) breast in Australia is used under specific circumstances. It is highly sensitive at diagnosing invasive breast cancer for tumours greater than 3-6mm in size. It does have a false positive rate of 12 % which means that areas which “light up” are 12 % of the time benign lesions.
It is useful in:
- Assessing dense breast tissue, and hence younger age groups.
- Assessment of a breast lump which presents with a normal mammogram and ultrasound. This particularly occurs in lobular carcinoma where it may not be seen, or the size is underestimated on conventional imaging.
- Assessment of leaking breast prosthesis
- Assessment of large T cell lymphoma associated with implants.
Once a lesion is detected, it requires a biopsy to confirm the diagnosis. Solid lesions should undertake a Core biopsy under the guidance of ultrasound or mammogram (otherwise called a stereotactic biopsy). This allows for the architectural assessment of the lesion. Fluid filled lesions can be assessed by a fine needle aspirate which only removes cells for assessment.
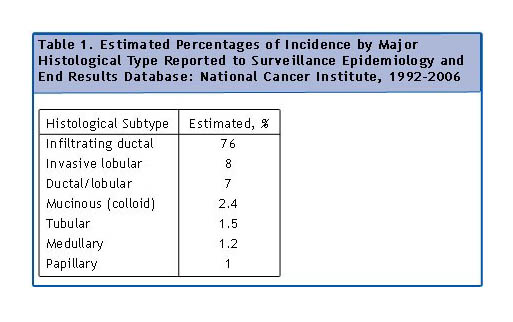
There are many types of breast cancer, with ductal (cells derived from the lining of the ducts) carcinoma being the most common (80%), and lobular the next. Invasive lobular (8-10%) tends to be bilateral, better prognosis, no microcalcification. Other rarer breast cancers are Paget’s (1-3%) and Inflammatory Breast Cancer.
Paget’s disease is a ductal carcinoma which invades the nipple associated with a scaling, eczematous lesion.
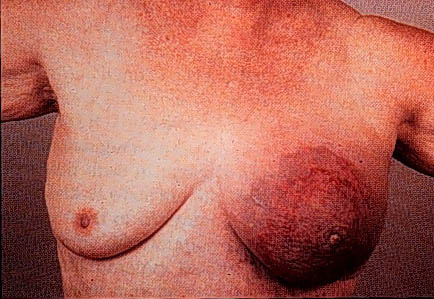
Inflammatory carcinoma (1-4%) a ductal carcinoma that involved dermal lymphatics. It presents with erythema, skin oedema, peau d’orange, warm swollen tender breast +/- lump. It tends to be the most aggressive of all the breast cancers.