A technique used to assess for small amount of cancer in the lymph nodes under the armpit (axilla) without having to remove all the lymph nodes (axillary dissection)
The sentinel lymph node(s) is the first draining node within a basin of approximately 20 lymph nodes. 85% of the breast drains to axillary lymph nodes.
Assessment of tumour in the lymph nodes is important as it allows control of the cancer just outside the breast prior to spread elsewhere in the body, and the ability to Stage the cancer for further treatment advice such as chemotherapy and radiation therapy.
It is located by injecting one or two dyes around the periareolar margin or around the the tumour site, just prior to surgery.
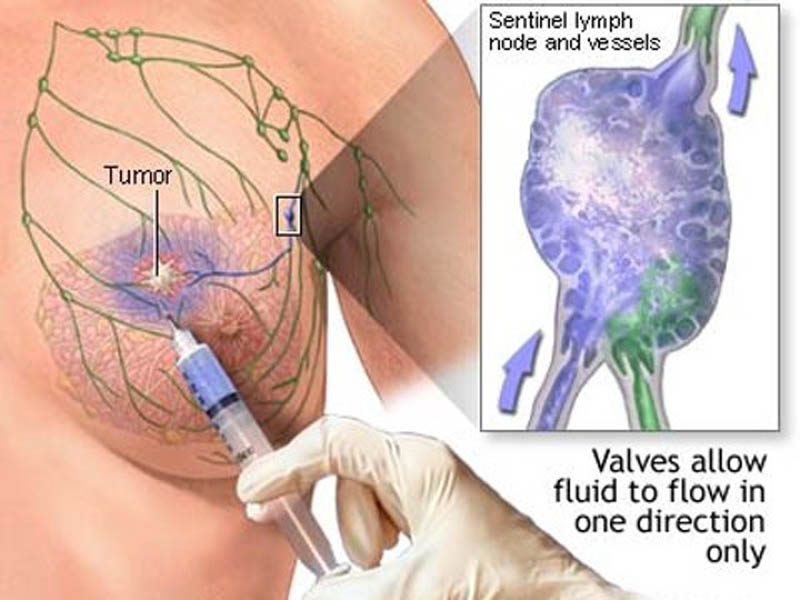
The dyes used are radioactive and patent blue dye, and the sentinel node is detected using a gamma probe to find a focus of radioactivity, as well as visually looking for a blue lymph node. There are now emerging techniques using a magnetic tracer to find iron particles, and visually looking for carbon particles.
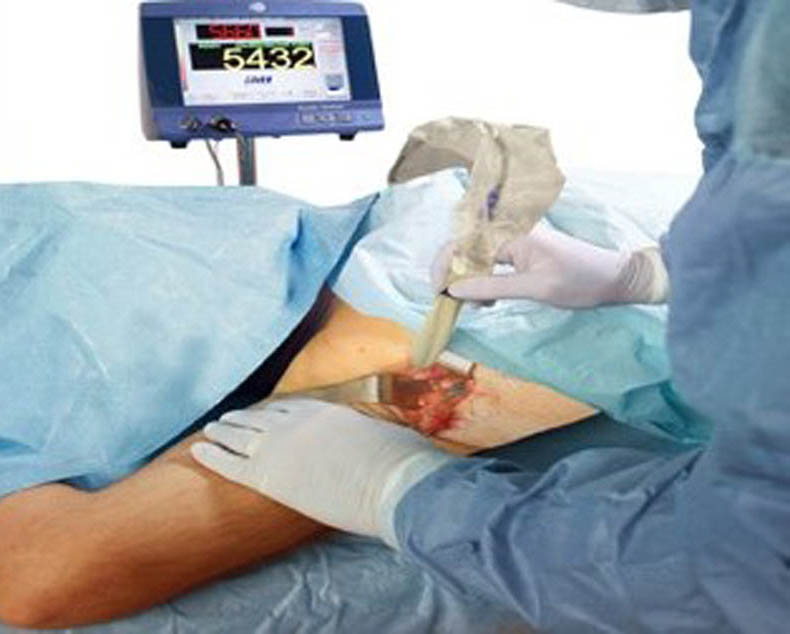
The sentinel nodes are checked for metastatic disease. Depending on the numbers involved and the size of the cancer deposit (> 3mm) the decision to complete an axillary dissection (removal of ALL the lymph nodes, within the axilla) is made.
Accuracy 97%. False negative rate 7%-12%. These figures can be obtained only by a surgeon well trained in this area.
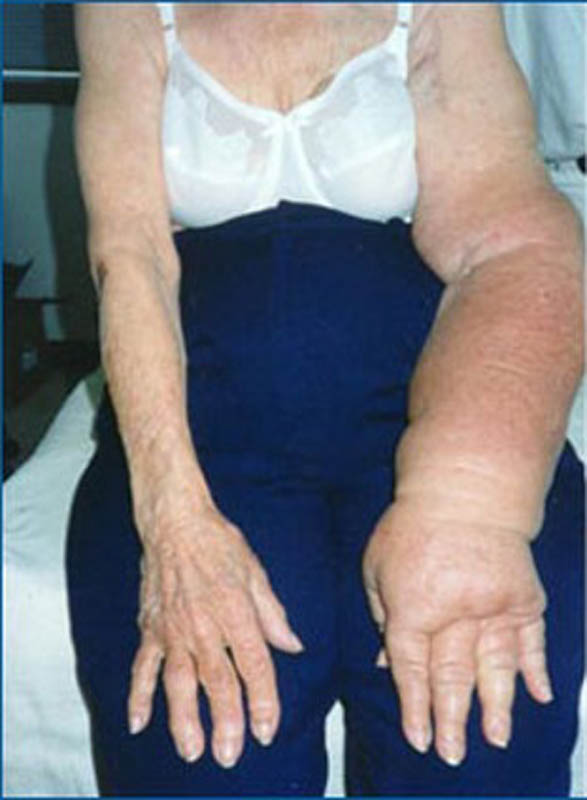
Sentinel node biopsy offers a significant decrease of complications commonly associated with an axillary dissection (removing all the lymph nodes). These complications may be seroma (fluid collection), lymphoedema (arm swelling), shoulder stiffness, parasthaesia (tingling and numbness of upper inner arm).
Procedure
Under general anaesthesia, inject the dye periareolar (around the nipple-areolar complex) during the actual breast surgery or prior as a single stand alone procedure.
Minimally invasive with either a small incision (1.5-2.5cm) under the armpit, or accessible through the breast incision for removal of the breast cancer.
Precise location can be achieved with little trauma to the surrounding tissue using the localisation techniques of a gamma probe and visualising the blue dye.
No drains required.
If performed solitary, only requires only a day stay. If performed in conjunction with breast surgery, follow post operative advice of the breast surgery.
Details
POTENTIAL COMPLICATIONS
- Bleeding Wound Infection Seroma (fluid collection) – minimal 4
POST OPERATIVE CARE
- Keep wound dry No driving / heavy lifting for 2 weeks
